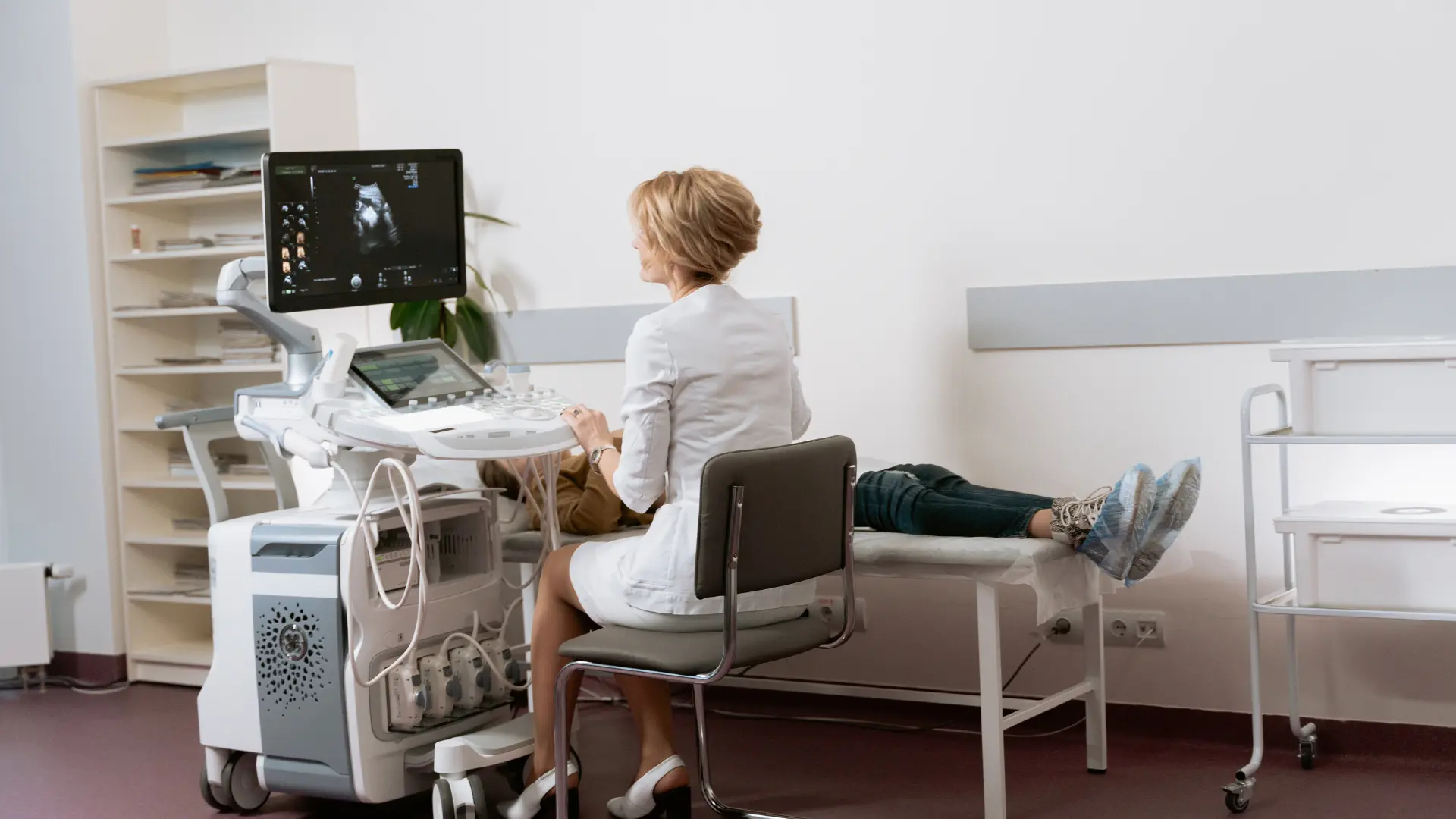
Every year in Switzerland, more than three thousand people die from lung cancer, the most deadly of all cancers. Men are the most affected, but in industrialized countries their tumors are decreasing, as many of them have given up tobacco. On the other hand, the number of cases increased among women who started smoking a few decades ago. The cigarette is indeed the enemy No. 1 of the respiratory system.
Late detection
There are two main lung cancers that differ in their rate of progression, prognosis and treatment. The “non-small cell carcinoma”, which is the most frequent (80% of cases), and “small cell carcinoma”. that is the fastest, most aggressive and hardest to cure because, when detected, there are always a few tumor cells that are already circulating in the rest of the body. Whatever their type, tumors are mostly detected very late. This explains why the five-year survival rate is overall 20% for women and 15% for men – whereas it can reach 60-70% if the tumor is detected at a very early stage.
The treatments used depend on the type of carcinoma and the stage reached by the cancer. If the tumor remains localized, it is eliminated by surgery or radiotherapy, sometimes accompanied by chemotherapy. This technique remains the only option in the most advanced stages, when there is metastasis.
In recent years, however, the therapeutic arsenal has expanded with the advent of drugs that target the tumor according to its biological profile. Some tumors, mainly non-small cell carcinomas, exhibit a genetic mutation that leads to the formation of an altered protein “inducing a crazy cell proliferation,”. The targeted treatments are therefore aimed at “repairing” this protein. Several drugs of this type are currently available in Switzerland. In people whose tumors have the target mutation, they are effective for one to three years. But then, the tumor finds the way to begin to proliferate and the cancer recidivates.
The greatest hope is, however, in immunotherapy, which aims to help our natural defenses to better fight cancer. Our immune system has weapons – white blood cells, called T-cells – capable of removing tumor cells. But if these are too numerous, it is overwhelmed by the task. Especially when the tumor is really malignant: when a T cell comes into contact with it, the tumor defends itself by disconnecting or by causing it to die. Immunotherapy therefore seeks to prevent it from doing so.
Treatments
Several immunotherapy drugs are already used in Switzerland. Reserved to patients – about one out of two – whose tumor has particular characteristics, they are then effective. Sixty percent of the people treated, most of whom had previously received chemotherapy, benefit from it, according to specialists. In 20% of cases, the tumor decreases in size and in others, it stops growing and stabilizes. “Surprisingly, tumors that were defending themselves the best way against the immune system and had the worst prognoses. are the most easily destroyed. In addition, unlike chemotherapy, immunotherapy does not attack healthy tissue and results in very few side effects.
Physicians also rely heavily on cell therapy. This technique, still experimental, consists of taking from the tumor of the patient T lymphocytes which are then “boosted” and cultivated in the laboratory and then reinjected into the blood of the patient. CHUV oncologists plan to launch a clinical trial in early autumn to test the efficacy of this method. It will be directed first to people with advanced melanoma and then, if it is conclusive, to those with lung cancer.