Pain treatment
After oncology rehab., relapse prevention
The benefits of our rehabilitation Restoring immunity Heavy metal detoxification Cleaning the body of the effects of chemotherapy Recurrence prevention To improve the patient’s well-being and

Blood and urine biocheckup
The biocheckup is a precocious diagnosis program focusing on the physiopathological imbalance associated with society illnesses. The precocious diagnosis of the metabolism imbalance at an

Treatment for cancer in Switzerland
Most cells in the human body are regularly renewed. Errors sometimes creep into this process. Normally, the cell corrects these errors or dies. When repair
Infertility treatment in Switzerland
According to the World Health Organization, infertility is characterized by the absence of pregnancy after twelve months of regular unprotected sexual intercourse. Causes and

DETOX Program
Detox is a deep cleansing of the body. Together with food, we get a lot of toxins in our body. Toxins have a negative impact

Treatment in Switzerland
Switzerland is the country with the most developed sphere of medical services in Europe. Our clinics are distinguished by high European standards of treatment in
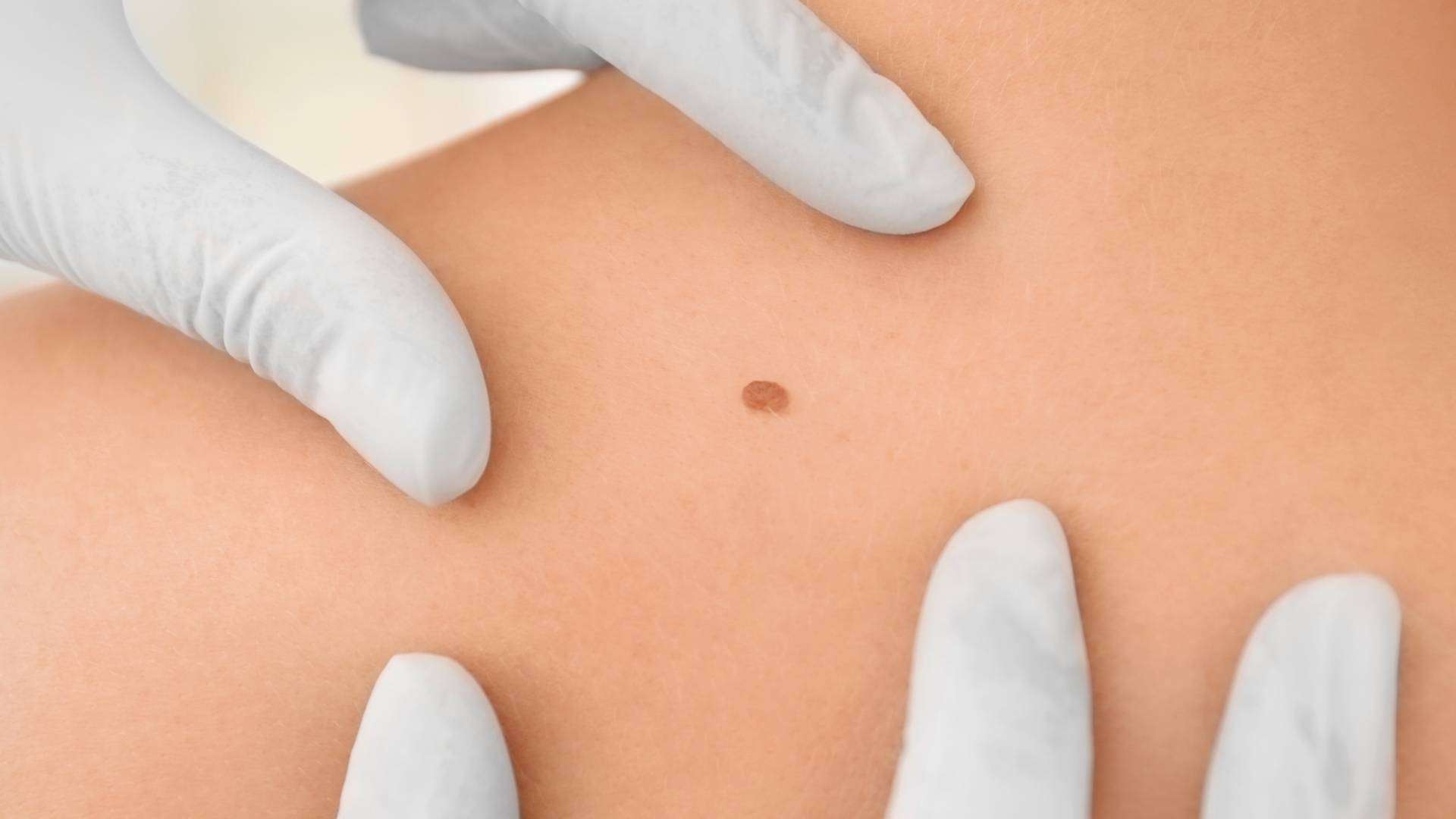
Skin cancer: symptoms, causes, treatment
Skin cancer is the presence of abnormal cells in the skin that multiply uncontrollably and form a carcinoma. Depending on the type of cancer, these

Duodenal cancer
The duodenum is the part of the digestive tract between the stomach and the small intestine. Duodenal cancer is very rare compared to stomach and
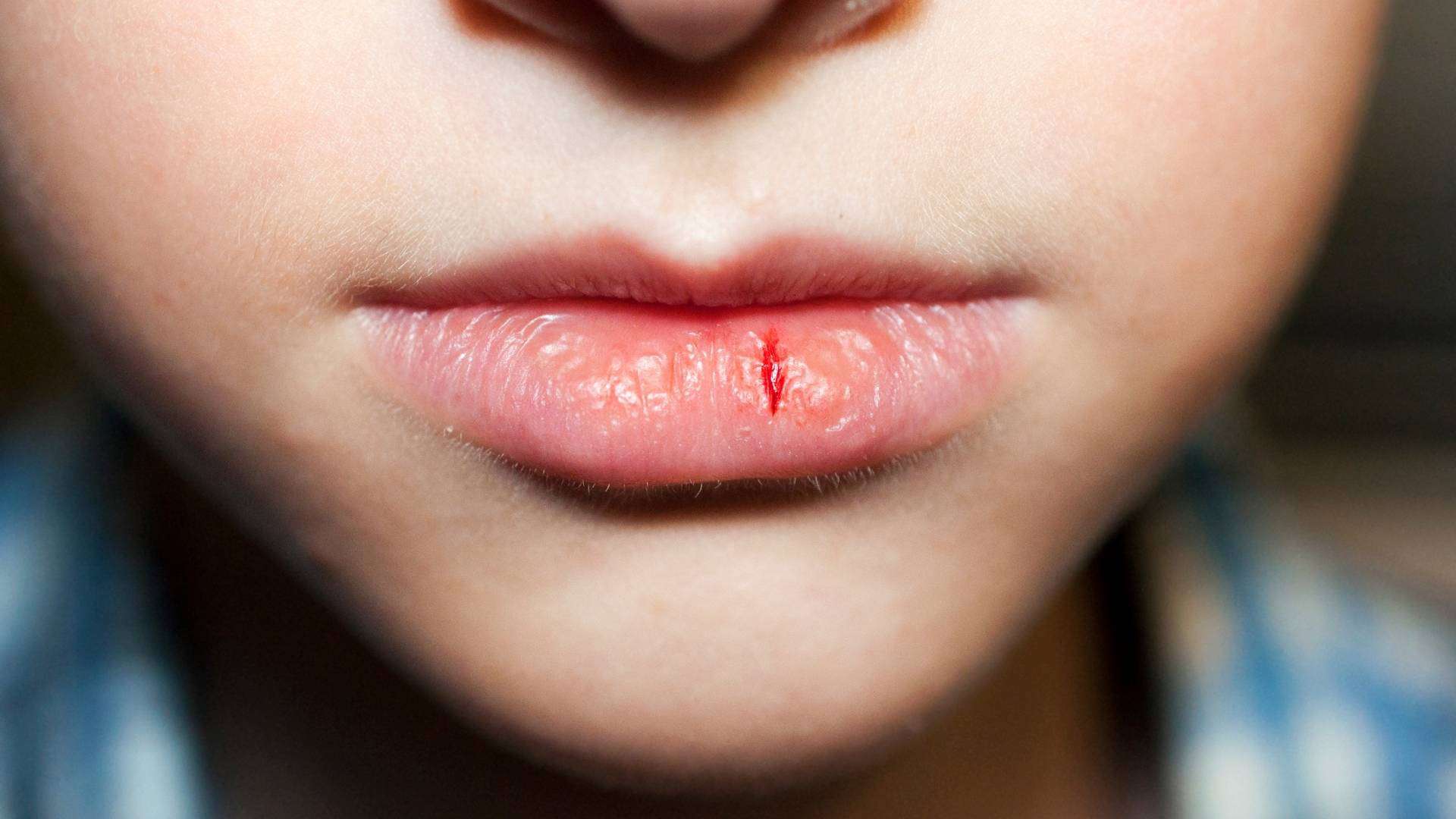
Lip cancer
The group of cancers of the upper digestive tract includes such diseases as lip cancer pharyngeal cancer salivary gland cancer larynx cancer cancer of the
