
Your DNA, Your Health
Your body holds an extraordinary amount of information about how you are built, which processes run faster or slower within you, and what you respond

Your body holds an extraordinary amount of information about how you are built, which processes run faster or slower within you, and what you respond

For a long time, medicine followed a simple principle: a disease appears — we treat it. Today, the focus is gradually shifting. We are talking
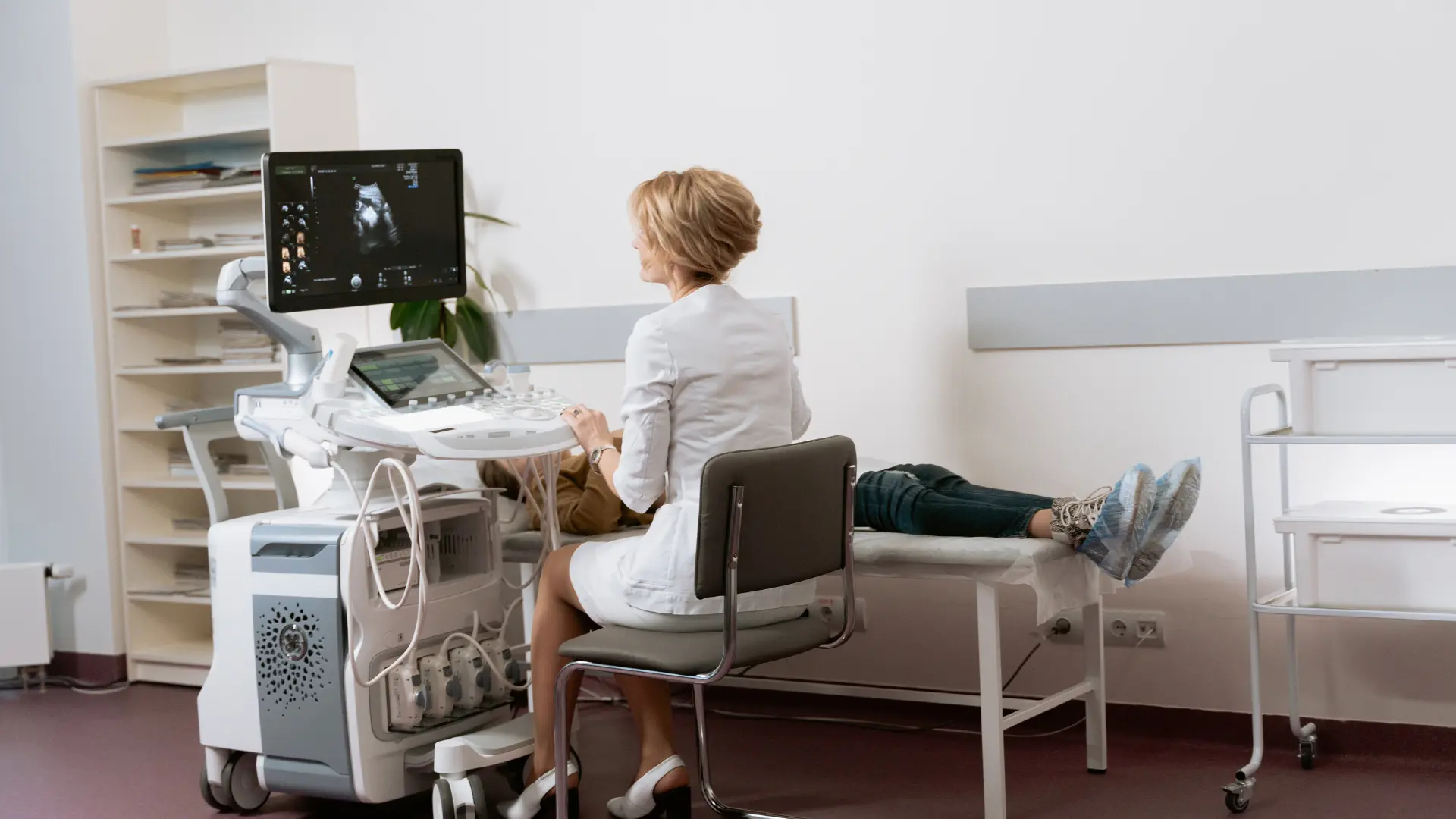
Many women view a visit to the gynecologist as a reaction to a problem: something hurts, unusual discharge appears, or the cycle becomes irregular. In

Hormones are the unseen regulators that govern nearly everything within the female body. Mood, energy levels, sleep, weight, libido, skin condition, and cycle regularity—all of

Essential oils are a wonderful gift from nature. Their scent soothes, energizes, helps with focus, improves sleep, and even supports the immune system. But behind

You go to bed on time. You drink coffee in moderation. You try to eat healthily. But you still feel drained by midday. Your thoughts

We all age. It’s natural. But why do some people look and feel 45 when they’re 60, while others, in their 40s, experience chronic fatigue,

Diabetes is not a sentence. It is a chronic condition that can be lived with fully, actively, and healthily. But only under one condition: you

Many couples dreaming of a child face difficulties when trying to conceive. Often, the first thought—especially in societies where it has long been assumed that

Imagine this: you immerse yourself in warm, clear water. Around you are mountains, silence, and a light mist hovering above the surface. The pressure of